This is part three of our series on the Five Mechanisms of External Accountability for Health Equity. Read parts one, two, four, and five.
Part 3: Transparency and Answerability
At the very core of accountability is the idea that you must operate in the light—making your actions easily visible to others—and must be able to tolerate some heat from stakeholders—answering for your choices, successes, and failures. These concepts of transparency and answerability are not deeply embedded in healthcare institutions’ approach to health equity, but moving forward they must be if these institutions are truly going to be held accountable for progress.
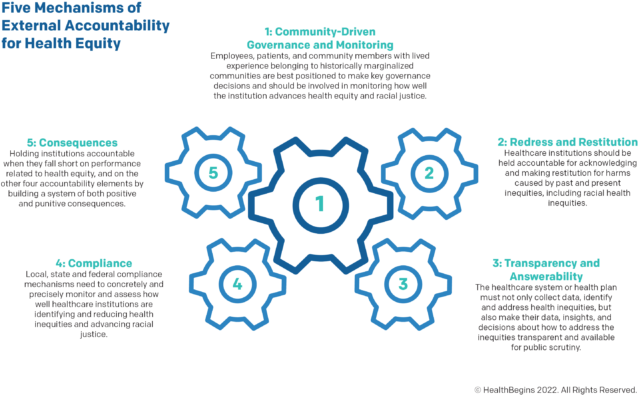
Transparency and Answerability is the third of the Five Mechanisms of External Accountability for Health Equity (see image below) examined in this blog series, and they are explored in-depth in this post.
Transparency starts with collecting and analyzing data that identifies health inequities as well as the impact of different programs and interventions on reducing those inequities. Then healthcare institutions must open up their health equity performance to public scrutiny by making that data available publicly.
As with all Five Mechanisms of External Accountability for Health Equity, how an institution engages with staff, patients, and community residents to answer these questions is, in many ways, as important as the decisions that are made. Moving toward stronger transparency and answerability cannot happen if the conversations about how to get there happen behind closed doors.
What Transparency & Answerability Look Like in Practice
More and more, healthcare delivery systems are collecting and analyzing direct, self-reported data on patients’ race, ethnicity, and language preference. The same goes for collecting patients’ social risk data. However, while social risk data is ostensibly used to inform efforts by population health management and community benefits teams, that same data is still rarely used to identify, analyze, and help reduce health inequities and advance racial justice. To truly be accountable for health equity, this data collection and analysis is critical.
Equally important is what is done with that data after it is collected. Institutions must publicize their data and decisions, particularly to members of communities historically harmed by societal and institutional practices and impacted by health inequities. Data analysts and healthcare executives cannot be the sole arbiters of what the data means or what steps are taken because of it. Sharing it publicly forces the institution to answer for its work and allows people outside the institution to both better contribute to solutions and hold the institution accountable for its progress or lack thereof. Below are examples of ways that some healthcare institutions have collected, analyzed, and publicly shared data explicitly to advance health equity.
Stratifying data to detect disparities in care
Intermountain Health in Utah developed dashboards that integrate data on race and ethnicity with data on patient outcomes so that the health system can see disparities across a variety of outcomes, clinical service lines, and locations. Similarly, Atrium Health in North Carolina created a tool to stratify data by race, ethnicity, gender identity, language preference, sexual orientation, and location. This Demographic Data Wall allows clinical leaders to identify disparities in health care, access, and outcomes. Some healthcare institutions publicize their data on health inequities through learning networks like the National Neighborhood Indicators Partnership and Data Across Sectors for Health to better understand how to capture and leverage this data. As health systems do better in stratifying data by these key demographics, incorporating social risk data—at both the individual and community level—is a key opportunity to better understand and communicate patterns of health inequity to patients and communities.
Communicating health equity data to drive patient-level care improvements
In 2019, after analyzing ten years of hospital data, physicians at Brigham and Women’s Hospital in Massachusetts concluded that Black and Latinx patients with heart failure were more likely than White patients to end up on the general medicine service rather than on the cardiology service, where patients have better outcomes. As one part of its Healing ARC program to address this inequity in care, the hospital shared its findings with focus groups from five neighborhoods with some of the highest populations of Black and Latinx residents and listened to residents’ ideas for a just path forward. Additionally, providers now acknowledge heart failure inequities with new patients at relevant points of entry into care. Other health systems have developed statistical process control techniques, such as run charts, to track measures more regularly over time, move beyond single-point dashboards, and inform continuous quality improvement.
Sharing health equity data to co-create community-level solutions
Collaborative Cottage Grove is a multi-sector health collaborative that mapped and rehabilitated more than 175 substandard housing units in a predominantly Black neighborhood in Southeast Greensboro, North Carolina. By doing so, they successfully reduced local emergency department admissions for childhood asthma. For its part, Cone Health contributed critical data that allowed asthma admissions to be mapped against city housing data. Cincinnati Children’s Hospital also participates in data sharing with a number of community-based organizations as part of a multi-sector health collaborative called Avondale Children Thrive. Together, they have created a place-based dashboard on child health and education outcomes in the city that helps drive social and structural health interventions to reduce health inequities.
Questions You Should Ask About Transparency at Your Healthcare Institution
To collect and data about health equity efforts, HealthBegins recommends finding opportunities to ask and discuss these questions about transparency at your healthcare institution:
- How does your healthcare institution collect and analyze patient data on race, ethnicity, and language (REL), sexual orientation and gender identity (SOGI), income, and location to identify patterns of health inequities?
- How does your healthcare institution collect and analyze patient social needs and community-level social determinants of health data (e.g., area-based social risk data) to better understand patterns of health inequities?
- How does your healthcare institution share data related to health equity and racial justice and make it available and accessible for public scrutiny in culturally and linguistically appropriate ways?
- How does your healthcare institution share and summarize trends and actionable insights about these identified health inequities and make these available for public scrutiny?
- Does your healthcare institution make financial and other essential records available to collaborating community representatives/organizations so they can independently evaluate the resources and staffing committed to services for communities impacted by health inequities, including BIPOC patients?
- How do institutional leaders provide a rationale for their decisions or actions taken (or not taken) to address identified health inequities? Do they make that rationale available for public scrutiny?
- How does your healthcare institution explain its decisions for actions taken (or not taken) to address identified social and structural drivers of health inequities at different levels of action (patient care, institutional practice, community, societal)?
By: Rishi Manchanda, Sadena Thevarajah, and Kate Marple
