This is part five of our series on the Five Mechanisms of External Accountability for Health Equity. Read parts one, two, three, and four.
Part 5: Consequences
Much of human behavior is driven by the proverbial carrot or stick; people are motivated by the promise of reward and the fear of punishment. Healthcare institutions aren’t all that different in this regard. It’s why there are a variety of positive and punitive consequences—such as awards and accreditation status—to enforce quality and safety standards in health care. Unfortunately, few of these consequences include health equity performance as a measure of quality.
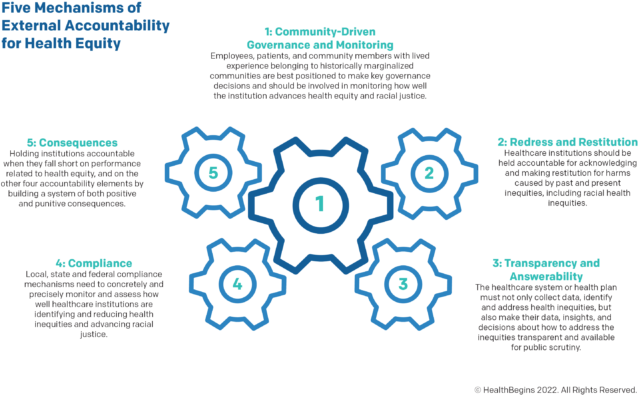
Healthcare institutions and health plans are rarely rewarded for actions that improve health equity outcomes, processes, or accountability systems such as community-centered governance, redress, transparency, and compliance. Similarly, healthcare institutions face little to no punishment when they fall short on reducing inequities in these same areas. Moving forward, creating these types of consequences is critical, and they are the final of the Five Mechanisms of External Accountability for Health Equity (see image below) examined in this blog series.
What Consequences Look Like in Practice
Below are different examples of how existing consequences could be modified and/or expanded to reward and punish health systems and health plans for their health equity performance.
Positive consequences
Recognition is one of the main ways outside groups reward health systems and health plans for their actions. Awards, such as the Malcolm Baldrige National Quality Award, celebrate work to advance quality care and safety. These types of awards could expand their criteria to include health equity measures as a marker of excellence.
The award that perhaps comes closest to elevating health equity performance is the Centers for Medicare & Medicaid Services’ CMS Health Equity Award. Created in 2018, the award specifically honors health systems and health care institutions that have reduced disparities and closed gaps in care. Each of the past winners identified specific racial health disparities among their patients—from colorectal screening to timely postpartum care to pneumonia readmission rates—and took steps that successfully closed gaps in care and outcomes.
Healthcare institutions are also incentivized and rewarded through payments, and these can be structured to favor reductions in health inequities. For example, Fairfax County, Virginia, worked with local safety net clinics to decrease disparities in cervical cancer screening, diabetes control, and hypertension control between Spanish-speaking patients, who had consistent access to on-site interpreter services, and the multilingual, non-Spanish-speaking patients who did not have access to these services. All members of the care team received a bonus for meeting quality of care and productivity measures, and higher fee-for-service rates paid for activities that promoted reductions in disparities.
Punitive consequences
While positive consequences can be helpful motivators, accountability cannot only be about giving gold stars. Health systems’ and health plans’ ratings, accreditation, and tax-exempt status must also be tied to their health equity performance.
The Joint Commission—the nation’s oldest and largest accrediting body in health care—currently identifies if hospitals collect race and ethnicity information, but it does not require that hospitals demonstrate improvements in health equity to meet standards of accreditation. Similarly, the Overall Hospital Quality Star Rating system—overseen by the Centers for Medicare and Medicaid Services—rates how each hospital performs on a set of five quality measures: mortality, safety of care, readmission, patient experience, and timely and effective care. None of the quality measures currently factor in a hospital’s health equity performance.
Every existing system that rates or accredits healthcare institutions should include reductions in health inequities as a quality measure. And to be truly effective, these assessments must look at more than data on health equity outcomes. Ratings and accreditation must also be used to strengthen the other accountability mechanisms for health equity by using community-centered governance, redress and restitution, transparency, and compliance as assessment criteria.
Prioritizing equity in how consequences are designed
It’s not enough to create health equity benchmarks that health systems and payers are rewarded for meeting and punished for when they fall short. To be both meaningful and just, equity must be prioritized in the creation and enforcement of these consequences. This means that they should seek to reduce structural inequities between institutions that disproportionately serve marginalized communities and those that do not. Healthcare institutions that serve disproportionately high numbers of people from marginalized communities often inherently rank lower on certain measures. This means that the data must account for that inequity, and that money must be invested in these places to level the playing field.
Questions* You Should Ask About Consequences at Your Healthcare Institution
*These questions are adapted from Dr. Bram Wispelwey and Dr. Michelle Morse’s article, An Antiracist Agenda for Medicine.
HealthBegins recommends finding opportunities to ask and discuss these questions about the internal and external consequences your healthcare institution faces for its health equity performance:
- What consequences from accreditation agencies, payers, and/or regulators does your healthcare institution face for identifying and improving (or failing to identify and improve) health inequities in patient care and outcomes?
- What consequences does your healthcare institution face for identifying and helping to improve (or failing to help improve) social and structural drivers of health inequity for your patients and community? Consider all of the following:
- Inequitable institutional practices, policies, and culture;
- Inequities in individual health-related social needs;
- Inequities in community-level social determinants of health; and
- Inequitable policies and structural forms of oppression or violence that disproportionately harm marginalized groups of patients and community members.
- Are there any community and state mechanisms, including reallocation of resources and/or fines, that hold your institution accountable to benchmarks of compliance with advancing racial justice and health equity?
- What internal consequences (both positive and negative) do institutional leaders, managers, and staff face for effectively implementing (or failing to implement) health equity and racial justice strategies? For example, is compensation tied to health equity performance?
While each of The Five Mechanisms of External Accountability for Health Equity serves a specific function, they produce stronger results when they work in tandem. Each one has the potential to not only hold health care institutions and payers accountable for health equity outcomes, but for how they pursue those outcomes. Community-centered governance is needed to make sure decisions about redress, transparency, compliance, and consequences are better informed by marginalized communities. At the same time, consequences are needed to reward and punish systems for how they include the voices of communities in decision-making, account for their past, open their work to public scrutiny, and create health equity benchmarks. Holding institutions accountable for reducing health inequities and advancing racial justice requires treating all systems as part of a whole.
By: Rishi Manchanda, Sadena Thevarajah, and Kate Marple
