Social needs: All
Patient population: 17,000 patients per year, 75% below the federal poverty limit, 83% Hispanic
Strategies: Medical-legal partnership
How it’s paid for: Grants, fellowships, federal dollars, and operating funds from a partner organization
Impact: Improved provider efficacy and satisfaction; quantitative impact analysis in progress
Advice for other upstreamists:

Keegan Warren-Clem
Managing Attorney
“My advice to an aspiring MLP attorney is: Lawyers — we’re problem solvers and law offers concrete solutions to the social determinants of health. Be persistent in educating yourself about public health and the terminology, and recognize where there are opportunities to take roadblocks that the medical community is experiencing and overcome those with solutions. So think concretely, think pragmatically, and then explore that in the language of these other professionals with whom you want to partner.”
Dr. Louis Appel
Pediatrician, Chief Medical Officer
“Be persistent. That’s really, really important. … There’s a lot of ups and downs to this kind of work, so keep the faith that if you keep working toward a goal you’re going to get over the ups and downs.”

Keegan Warren-Clem and Dr. Louis Appel’s story:
When a patient at People’s Community Clinic in Austin, Texas, needs something more than routine care, her provider can refer her to the typical roster of specialists: a cardiologist, an orthopedist, a gastroenterologist. Plus one that’s far less typical: a lawyer.
That lawyer is not an outsider from another organization, not a visiting volunteer holding office hours in the clinic conference room. She is a full-fledged clinic staff member who sees patients in an exam room, as much a provider as any nurse or doctor on the team. The patient can schedule an appointment with her at the clinic’s own front desk.
Medical-legal partnerships (MLPs) are growing more common around the country. The National Center for Medical-Legal Partnership counts nearly 400 such programs in the U.S.
But People’s Community Clinic brings this kind of integration to the next level. The MLP providing legal care at the federally qualified health center, which serves 17,000 patients a year, has four full-time lawyers, with a fifth joining this fall. And those lawyers are integrated so fully into the clinic’s policy and practice that they might as well wear white coats as business suits.
With a partnership that integrated, “you have a tool that can be the difference between having a home and not having a home,” says Ellen Lawton, co-director of the National Center for Medical-Legal Partnership. “It’s the difference between being deported and not being deported. The difference between having your Social Security check and not having your Social Security check. It’s literally that dramatic.”
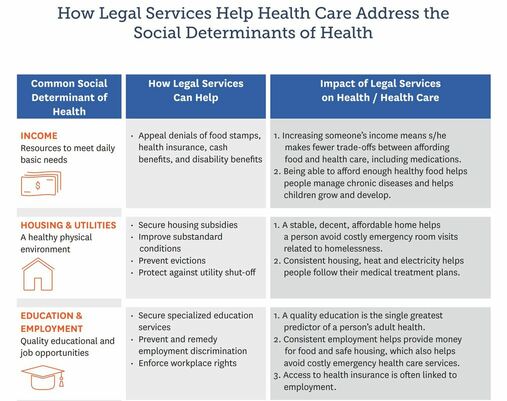
From Outsider to Provider:
The People’s partnership began in 2012, when two puzzle pieces clicked together. The clinic’s Chief Medical Officer, Dr. Louis Appel, a pediatrician with an interest in addressing the social determinants of health, and clinic CEO Regina Rogoff, a lawyer and former executive director of Legal Aid of Central Texas, had been trying to start an MLP but struggling to find funding and convince their board that legal care wasn’t mission-creep. Keegan Warren-Clem was a new law school graduate with an Equal Justice Works Fellowship, via the nonprofit Texas Legal Services Center, to start an MLP in Austin. All she needed was a place to do it.
When the three met, the match seemed obvious.
Despite the administrators’ wholehearted support, logistics and traditions set the program up for a slow start. Warren-Clem began as a clinic outsider trying to make her way in. She worked out of an office in a separate building, paying visits to providers with a 10-item screening questionnaire and a laminated information card.
The program has since evolved in essential ways. Warren-Clem, as well as two additional full-time lawyers, has her office right in the clinic. A single, universal screening questionnaire (which the lawyers helped develop) checks for unmet health-related legal and social needs. Referrals to legal care are made through the exact same system as referrals to medical care. And medical and select legal information are embedded side by side in patients’ electronic health records.
Paid protected time for “clinical champions” — originally three and now 13 staff members ranging from physicians to social workers to receptionists, who identify and address challenges within the program — has also helped the collaboration take root.
Where Warren-Clem once struggled to compete for providers’ attention, she and her fellow lawyers now provide seamlessly integrated, individualized legal care.
In one case, a 6-year-old girl was suffering recurrent asthma attacks, triggered by cigarette smoke entering her home from the apartment next door. Building managers had told the family they had no recourse, as smoking was allowed in the apartments — until clinic lawyers intervened and convinced the managers to allow the family to break their lease and move.
Pediatrician Dr. Sandra Frasser remembers another time when a mother told her she had to tape up her bathtub with duct tape to keep a flood of water from leaking out with every shower. The dampness had drawn rats, but property managers hadn’t fixed the problem. “It just made me so angry hearing her story,” Frasser recalls. “Once I referred them to Keegan, it was just a matter of her writing a letter to the management and suddenly it got fixed.”
Each lawyer other than Warren-Clem, who manages the program and focuses on adults experiencing chronic pain, specializes in a particular population: prenatal and postnatal mothers, LGBTQ+ patients, and adolescents. Their work with patients ranges from advice to full representation in court. Yet their role at the clinic also extends broadly into practice and policy. The lawyers’ services include:
- Collaborative care. For example, the lawyer who specializes in maternal health, Daphne Wilson, co-facilitates group prenatal visits with a nurse-midwife. “Let me say that again,” says Warren-Clem. “It’s a nurse-midwife and an attorney, and they’re doing these visits together, all of them.”
- Staff training. Lawyers regularly give presentations to educate medical staff about health-related legal needs, improving their general knowledge and the precision of the referrals they can make.
- Practice transformation. For example, the legal and medical staff worked together to design a new system for tailoring medical decision-making plans for minors turning 18. The lawyers also recently helped develop the clinic’s new pain-management protocol.
- Community education. Lawyers regularly provide know-your-rights sessions to address health-harming legal needs in the community. For instance, Wesley Hartman is in the midst of a series about law and gender.
- Outside partnerships. Warren-Clem helped develop a partnership with the Austin Tenants Council. A regular workflow now enables providers to refer patients directly to the council if their housing needs fit certain criteria. Christopher Sailer is working to develop relationships with educators to address the needs of students, a tactic that Kassandra Gonzalez hopes to build upon when she joins the team later this year.
- Legislative advocacy. Staff advocated publicly for a paid sick leave ordinance that the city of Austin ultimately adopted. They also entered public comment on proposed changes to the federal “public charge” policy, which would deny green cards to immigrants who have used public benefits such as housing assistance, food stamps, or Medicaid.
The Route Upstream:
For both Appel and Warren-Clem, the epiphanies that led to the medical-legal partnership began long before the partnership itself.
“One night during medical school I was sitting in a hospital admitting two patients, and they each had a stack of charts literally a foot and a half tall,” Appel remembers. “And I decided at that moment that that was not really what I wanted to be doing.” Instead, Appel wanted to start healing patients before their illnesses became so entrenched, so he gravitated toward pediatrics and upstream care.
Warren-Clem had taught high school Spanish, a role that gave her a vivid view of students’ unmet social needs. While in the Army National Guard, she recognized a gap in support for families of service members being sent overseas, so she started a nonprofit to provide that. But it was in law school when her vision of how defending people’s wellness set them up for life success really crystallized.
As a student intern at Texas Legal Services Center, she took on the case of a young man who had become unable to regulate his emotions after a traumatic brain injury suffered in youth sports. A trial of a particular drug corrected the problem — but his insurance refused to cover a prescription. His medical care team appealed the decision, but it was “completely outside the realm of what any physician would be trained in,” Warren-Clem says. “And it just struck me: Why are we asking physicians to do this anyway?”
In the end, Warren-Clem got the drug denial reversed and set a precedent that ultimately changed the FDA regulation behind it. To that young man and his family, she says, access to the drug meant “everything. Because to be socially appropriate is what allows us to have friends, to be ‘normal’ in various environments.”
For the young lawyer herself, she adds, “That was really it for me, this example of work that was really much better handled by an attorney that would have a positive impact on health for both individuals and an entire population.”
Lessons for Sustainability:
Despite the program founders’ passion, sustaining the MLP at People’s Community Clinic has not been simple.
A funding gap forced a temporary suspension of the program in 2014. Since then it has run on a mix of funds, including regular operating dollars from Texas Legal Services Center, a grant from Episcopal Health Foundation, a fellowship from Equal Justice Works, and Health Center Expanded Services Supplemental Funding from the federal Health Resources and Services Administration.
The clinic’s board of directors is now fully convinced of the program’s value, says Dr. Appel: “Having the MLP did help move everybody’s thinking a little bit about what the clinic’s role is.”
The National Center for Medical-Legal Partnership tracks growing evidence that MLPs can reduce hospital admissions; improve adherence to treatment plans; reduce spending on high-need, high-cost patients; improve patients’ mental health. People’s also is working to build its own impact data. The clinic recently embedded legal data into its EHR system and aims to match geographic, health, and legal information to see a comprehensive picture of associations.
Personally, both lawyers and medical staff at People’s find the collaboration essential — a symbiotic relationship that allows people in both fields to do their best work.
“There are so many things that impact people’s health that are outside of the strictly medical issues that we can directly address in the exam room … and you feel not only ineffective if you can’t address those, but it can be frustrating,” Appel says.
Warren-Clem, for her part, says, “My practice is fun and it’s easier and it is creative because I get to work with medical experts. What that means is we are able multiply our frontline capacity as attorneys by leveraging the expertise of providers and using that to improve outcomes for patients.”
Case in point: People’s Community Clinic cared for an older couple in which one partner had cancer. They were also victims of a cruel yet completely legal predatory lending scheme that had them paying nearly 64 percent interest — a strain that drained their capacity to afford chemotherapy and put them under severe, health-sapping stress. The patient’s physician put in writing the impact on the couple’s health, “and we actually took that to the judge, and with hands wide open said, ‘This is the real-life impact of this case,’” Warren-Clem recalls. “We couched it in legal arguments as much as we could, but it worked.”
The court approved the dismissal of the case.
“We couldn’t have achieved that outcome without having providers on the legal team,” says Warren-Clem. “So for me this is also a better way to practice law.”
One of the key lessons from People’s, says the National Center’s Lawton, is to build a unified, shared vision that is not about either law or medicine, but about health. Another lesson is to admit mistakes along the way, adapt, and stick with it.
“People think you’re going to flip a switch, turn the lights on, and an MLP appears,” Lawton says. “Austin’s experience is this takes time, it takes leadership, it takes persistence and passion. … Look at the Austin story and see what impact you can have, and take your vitamins and settle in, because it’s going take a while, but it’s going to be worth it.”
The National Center for Medical-Legal Partnership’s origin story on Austin People’s Community Clinic helped inform this report.
To learn more from additional examples of medical-legal partnerships, check out the “Patients to Policy” series from the National Center for Medical-Legal Partnership.
Learn how HealthBegins can help you move healthcare upstream. Contact us to learn more.
Featured Content
Why DEI Matters for Health Equity—And How to Protect It
Diversity, Equity, and Inclusion (DEI) is a critical element of health equity, but around the country we continue to see coordinated efforts to dismantle DEI in all settings. In this post, Natashia Townsend recounts how she helped preserve DEI initiatives in her home state of Arizona and what...
How to Read the New Federal Dietary Guidelines as a Health Equity Advocate
The new Dietary Guidelines released by the Department of Health and Human Services not only run counter to established health standards, but also against health equity goals. Here are the the issues with these guidelines and what actions health equity advocates can take for better outcomes.
Small Practices Improve Health and Health Equity in Big Ways
The EQuIP-LA effort led to statistically significant health improvements and highlighted lessons that could help amplify the impact of small practices in advancing equity in more places.



